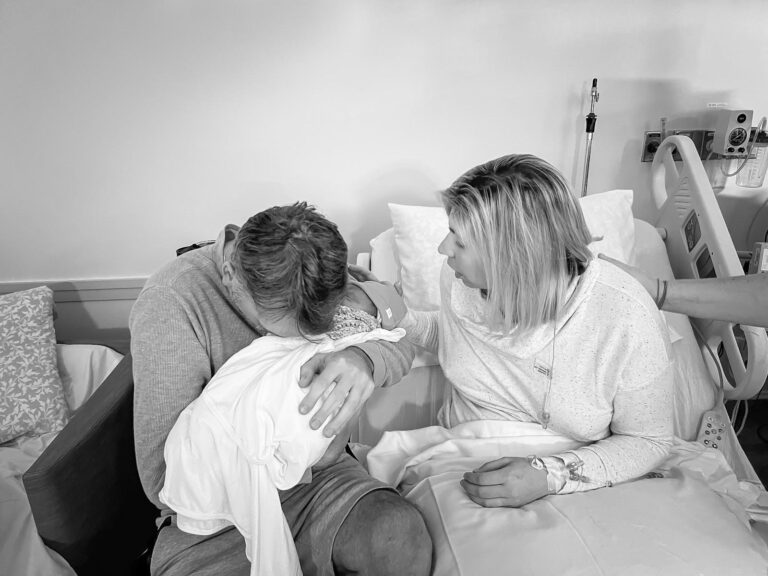
by Jennica Hill
I want to tell you about Hugo.
Recently, I watched a television show representing a true story about a woman who died of breast cancer. When she died, I cried. I cried for her, of course, for her friends and family, for the thought of losing loved ones and for the loved ones I have personally lost to cancer. But, above all, which might seem strange, I cried for Hugo.
Hugo is my son whom I never got to meet alive. My son who died inside my body and whose body I gave birth to at 39 weeks–one week before his due date. I thought about how, even if he were to get cancer as an adult like this woman did, at least I would have seen him live. I wanted to see him live. I wanted to be part of that life. Instead, what I got were nine months of feeling his abstract, insistent movements inside my uterus. I got to love him from afar, even though he was right there the whole time. And what some may never realize because they just don’t understand the impact of stillbirth: I will love him every day of my life. I don’t know what I believe about the afterlife, but I do hope he’s in mine. I just want to have a cup of coffee with him. I want to see him get married or even go through a break-up. I want to see him do anything but die. Missing him hurts my entire body. This is the kind of pain that stillbirth causes. This is the kind of pain that so often goes unnoticed or silenced. Please don’t shy away from my pain, and please help me prevent others from going through it, too.
Because Hugo’s death was preventable. Throughout my “low-risk” pregnancy, I had a feeling something was wrong, even though I had no evidence to support my fears. I was sad and scared, even through the giddiness of looking forward to meeting my first baby. I did find out he was breech near the end of my pregnancy, and I thought that was the thing that might break me, as I worried about having an unwanted surgery. But the thing that broke us both was that he had a small placenta, which went undetected because measuring estimated placental volume is not part of standard prenatal care in the United States. Finding this out has been a journey, and I had to do the vast majority of research myself, while in the throes of my deepest grief.
After my husband and I received Hugo’s autopsy report from the hospital, the obstetrician who helped deliver Hugo told me there was “nothing exciting” on the report and that Hugo was a “healthy baby.” He said this would likely never happen again. Not only did this seem like an insensitive choice of words and strange considering Hugo had died, but my intuition also told me something went wrong that could happen again. So, after learning about the organization PUSH for Empowered Pregnancy from a fellow loss mom, I sought answers from Dr. Harvey Kliman, a research scientist at Yale Medicine specializing in infertility and pregnancy complications, including pregnancy loss. Though my insurance would not cover his analysis–another conversation for another time–I had Hugo’s placental slides sent to Dr. Kliman, and he told me Hugo’s placenta was too small to sustain him at the end of my pregnancy. The baby’s placenta acts like the roots of a tree and provides the baby with the nutrients and life-force they need to survive until birth. While Hugo’s body was in the 30th percentile, his placenta was in the .99th percentile. I learned babies’ bodies should have a 6:1 ratio with their placentas, while Hugo was trying to survive with a 30:1 ratio. Dr. Kliman explains a death like this as akin to the gas running out of a car: it’s sudden, and the only way to prevent it is to detect that something is wrong beforehand. I had been to the OB the day before Hugo died, and everything seemed fine, so the only way I could have known he was struggling was to have an ultrasound tech perform a quick measurement to determine Hugo’s EPV, or estimated placental volume.
To so many medical professionals, stillborn babies are a statistic, one they can gamble with knowing they might only encounter a horrible loss like this once every few years. It’s not that I blame them, and I’m sure they don’t see it the way I do: I understand they have to do their jobs to the best of their ability with the knowledge they have. Caring for pregnant people and fetuses must be full of terrifying possibilities. No one wants to get sued. But, if we know placentas keep babies alive in utero, why are we not doing everything we can to measure them and keep them healthy?
I want you to know something else. I didn’t just lose my baby; I lost myself. Once a vibrant, perhaps overly productive young woman–I yearned to lift the spirits of everyone I met–I am now flattened by the death of my enigmatic first baby. He’s as much a mystery to me as he is to most, though I’m the only one who truly felt him while he was alive. Maybe someone will read this and feel bad for me, feel bad for the roughly 65 sets of other parents in the U.S. who gave birth to stillborn babies on October 21, 2021 and the over 20,000 babies stillborn every year in the U.S., but my fear is that no one who can make a difference will feel bad enough to take action (CDC).
Perhaps because I searched for and found answers about Hugo’s death, I have since given birth to two beautiful living sons. I am so grateful, but throughout my rainbow pregnancies, or pregnancies after loss, there were medical professionals who dismissed Hugo’s death, my anxieties, and my insistence that they measure my babies’ placentas. An OB who would have cared for me had my midwife been unable to when I gave birth to my first living son even told me I’d had “a bad spin on the roulette wheel” when Hugo died and that, odds were, my second son would live. My first son is not a spin on a roulette wheel, and as much as I adore my living sons, having them does not negate the constant missing Hugo and the inability to ever make the memories I so vividly imagined while pregnant with him. I also now know that, according to the NICHD, parents who have had one stillborn baby are more likely to experience the same traumatic loss again.
To help prevent stillbirth, we need more research to support changes in prenatal care, like measuring babies’ placentas. We need providers to bravely adopt these changes, even though they might incur additional risk in doing so. We need everyone involved in prenatal care in the United States to join other high-income nations in their efforts to reduce stillbirth. According to PUSH for Empowered Pregnancy, 75% of stillbirths could be avoided if the United States matched the work of the most successful nations. In Georgia alone, about 8 of every 1,000 live births end in stillbirth. And non-Hispanic Black mothers experience stillbirth at double the rate of their white counterparts. None of this okay. None of this should be acceptable. But the decline in stillbirth rates in the United States has remained the same in recent years, despite constant medical advances. We need to do better.
Most mothers and fathers fear the death of their children and look for every possible danger. But the truly unlucky ones know what it actually feels like when it happens. And then there are those of us who not only held our dead children but also birthed their bodies first, going through the pain of childbirth to endure a much worse pain immediately after as we look into the beautiful face of a child whose eyes and smile we will never see. I know there are some stillbirths that, devastatingly, cannot be prevented. But Hugo’s death and the death of 1 in 4 of stillbirths in the U.S. every year can be (PUSH for Empowered Pregnancy). Please stand with me to prevent these deaths. Stand with me to help other families avoid the lifetime of pain mine and so many others face.